We use cookies to make your experience better. To comply with the new e-Privacy directive, we need to ask for your consent to set the cookies. Learn more.
What is PCOS?
PCOS stands for polycystic ovary syndrome. It affects around 10% of people with female reproductive organs and is one of the leading causes of infertility.
What are ovaries?
Here's a simple diagram of the female reproductive system—remember, every body is different, but this gives a pretty good idea of what's going on for many people with ovaries.
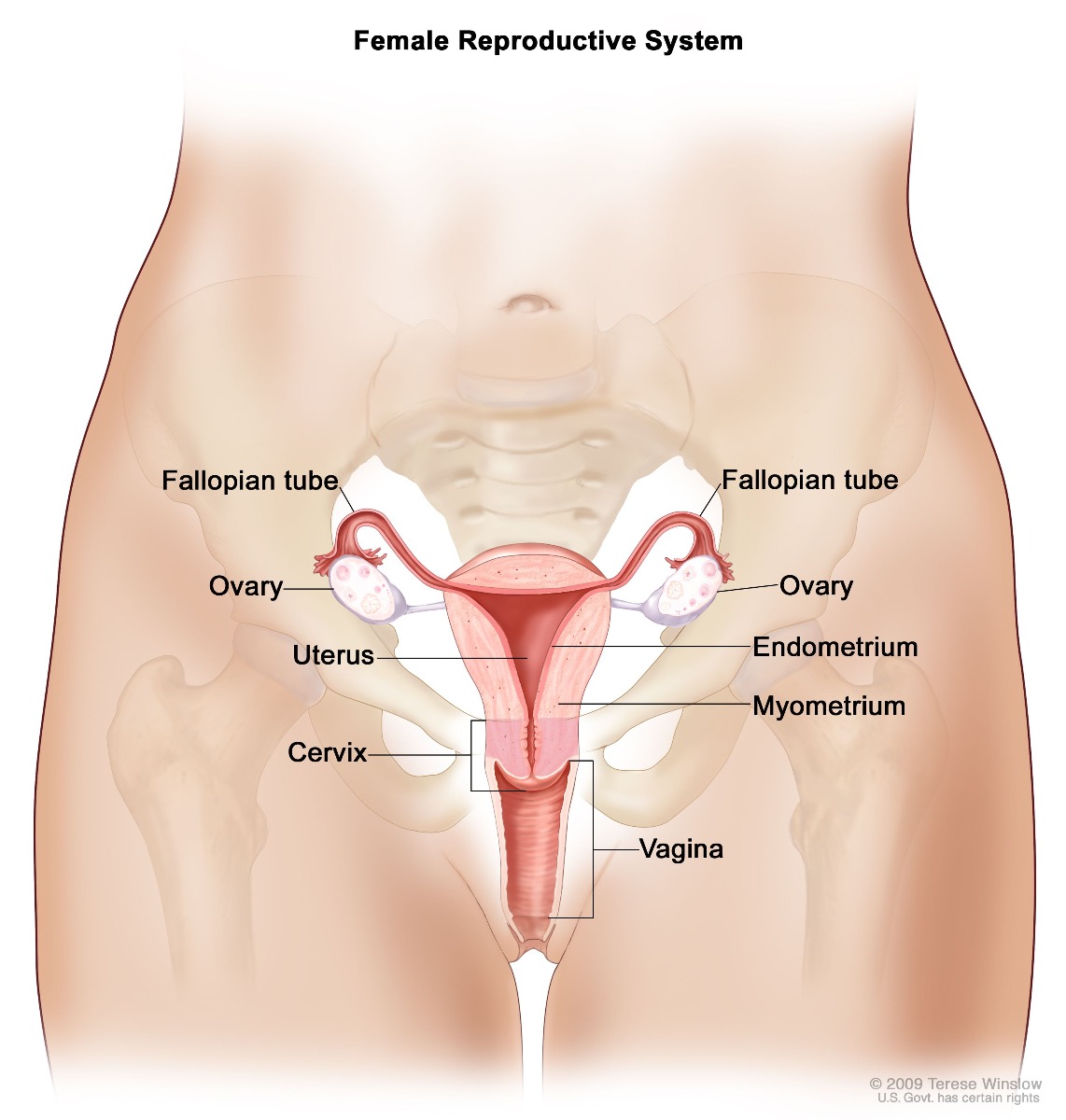
There are two ovaries on either side of the uterus, which are around 4 cm long. Ovaries are small glands where the eggs (the 'ova') live and where estrogen and progesterone are produced. People with female reproductive organs are born with all the eggs they will grow in their lifetime. These eggs are protected by a layer of cells called follicles.
Ovulation happens in the first phase of the menstrual cycle. During ovulation, the eggs start to mature, and the follicles grow larger and produce estrogen. When a follicle and egg are ready, the follicle releases the egg into the fallopian tubes. At this stage, the follicle becomes the 'mature corpus luteum', which produces higher levels of progesterone (during the second phase). This causes the endometrial lining of the uterus to thicken. If the egg finds any sperm, then it may be fertilised and lead to pregnancy. If there's no pregnancy, the body will release the egg with the endometrial lining during a period. The menstrual cycle then starts all over again.
What causes PCOS?
PCOS is a 'syndrome' that is characterised by a group of symptoms affecting the ovaries and ovulation. The exact cause of PCOS is not known and diagnosing it can be difficult.
PCOS gets its name from the growth of cysts in the ovaries. When the follicles are growing larger to support their eggs, they can sometimes stop growing and fail to release the egg. When this happens, the enlarged follicles are considered ovarian cysts. A build-up of cysts in an ovary can eventually cause enlargement of the ovary.
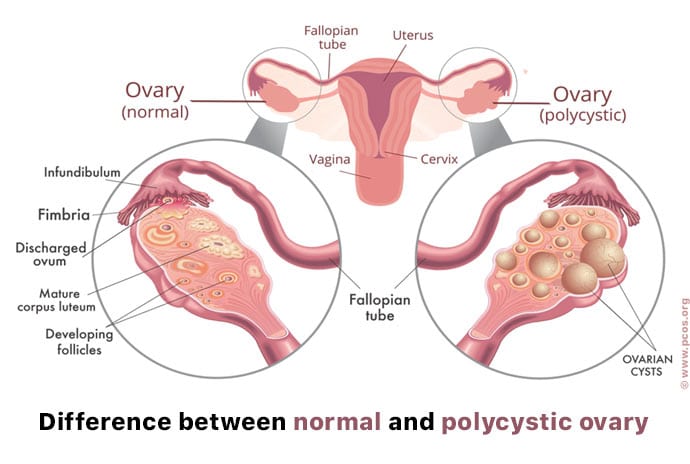
PCOS often runs in families and is related to abnormal hormone levels, including high levels of insulin. People with PCOS can be resistant to the action of insulin in their body, and they may produce even higher levels of insulin to overcome this. As a result, the ovaries might produce heightened levels of male hormones (mainly testosterone). If people with PCOS are overweight, then they may also experience increased insulin production. This is a bit of a nightmare because insulin controls sugar levels in the body. The side effects can affect a person's appetite, mood and sleep patterns.
What are the symptoms of PCOS?
It's estimated that 1 in 10 people with ovaries experiences PCOS (in the UK). More than half of these do not have any symptoms. However, the other half might experience the following:
- irregular periods or no periods at all
- difficulty getting pregnant because of irregular ovulation or failure to ovulate
- excessive hair growth (hirsutism)—usually on the face, chest, back or bum cheeks
- weight gain and difficulty losing weight
- thinning hair and hair loss
- oily skin or acne.
How is PCOS diagnosed?
Because of the varying nature of the symptoms, it can often take a long time to diagnose PCOS. For a diagnosis of PCOS to be confirmed, other hormonal conditions must first be ruled out. Then, at least two of the following symptoms must be present:
- irregular or non-existent periods
- increased male hormones, shown by excess body hair or blood samples
- multiple cysts in the ovaries found during an ultrasound scan.
What are the long-term effects of PCOS?
PCOS is associated with an increased risk of developing health problems later in life, such as type 2 diabetes and high cholesterol levels. People with PCOS are also at a higher risk of developing heart disease, high blood pressure, sleep apnoea and strokes.
If a person doesn't experience a period for a long time, this can cause problems with fertility. There is also evidence that a prolonged build-up of the endometrium can increase the risk of endometrial cancer. However, this risk can be managed by using treatment methods to ensure that the endometrial lining is shed at least once every 3 months.
Is there a cure for PCOS?
Unfortunately, there is no cure yet. The good news is it can be treated, and some people have even reversed their symptoms. However, it takes some real dedication and self-monitoring, which can be challenging at the best of times.
There are many treatment options available. These include medicines like Metformin or specific types of contraceptive pills, or more natural choices, such as dietary changes and exercise.
It's important to consult a medical professional to seek the correct treatment for your specific circumstances.
If you experience irregular periods, excessive acne or hair growth, or are having trouble getting pregnant, then talk to a medical professional (such as a GP) about PCOS. If a diagnosis is confirmed, ask your GP to also run a test for type 2 diabetes.
Over 20,000 people have shared their experiences with PCOS:
https://www.stuffthatworks.health/pcos
Some nutritionists with knowledge about PCOS:
https://www.salenawalker.earth/
https://www.taschmarholistichealth.co.uk/
YouTube: Prof Lusting, Dr Ken Berry, Dr Rob Cywes and Dr Boz
Audible/book: The PCOS Plan by Jason Fung
Written by Charlotte Smith and Nina Giblinwright.
Edited by Nina Giblinwright.
